Author: Kashif Rauf
INTESTINAL ISCHEMIA
Intestinal ischemia results from occlusion of arterial inflow, venous outflow or failure of perfusion resulting in abdominal pain called abdominal angina.
1. Arterial inflow occlusion
2. Venous outflow occlusion (Mesenteric vein occlusion)
3. Failure of perfusion
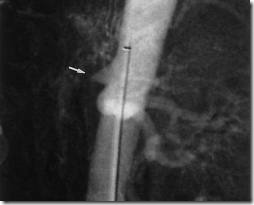
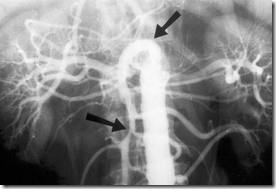
Mesenteric Vein occlusion
Diagnosis is made with contrast CT or angiography.
Treatment is long-term anticoagulation. Surgery is reserved for bowel infarction.
INTESTINAL ISCHEMIA
Intestinal ischemia results from occlusion of arterial inflow, venous outflow or failure of perfusion resulting in abdominal pain called abdominal angina.
CAUSES OF INTESTINAL ISCHEMIA
Intestinal ischemia may result from any one of the following causes;1. Arterial inflow occlusion
- Atheroma ( Read About: atherosclerosis, risk factors, Causes and Atheroma formation )
- Thrombosis
- Embolus
- Aortic disease
- Vasculitis e.g Takayasu’s arteritis
- A tumour (causing compression of the vessel)
2. Venous outflow occlusion (Mesenteric vein occlusion)
- Hypercoagulable states e.g malignancy,
- protein C, protein S, or antithrombin III deficiency).
- Antiphospholipid antibody
- Intraabdominal sepsis
- Portal hypertension and cirrhosis
3. Failure of perfusion
- Hypotension, shock
Acute small intestinal ischemia
- An embolus from the heart in a patient with atrial fibrillation is the commonest cause, usually occluding the superior mesenteric artery.
- Patient presents With sudden abdominal pain and vomiting. The abdomen is usually distended, tender and bowel sounds are absent. A patient is hypotensive and ill-looking.
- Angiography may be performed in a stable patient and thrombolytic therapy (alteplase) may be given for thrombotic disease,
- For unstable patient treatment is usually laparotomy with thromboembolectomy and resection of gangrenous bowel Antibiotics are given to all patients. Mortality is high.

Chronic small intestinal ischemia
- This is due to atheromatous occlusion or cholesterol emboli of the mesenteric artery, particularly in the elderly.
- Patient presents with abdominal pain occurring after food. Acute mesenteric occlusion may develop chronic occlusion.
- Diagnosis is made with angiography.

Mesenteric Vein occlusion
Diagnosis is made with contrast CT or angiography.
Treatment is long-term anticoagulation. Surgery is reserved for bowel infarction.
Ischemic colitis
- Occlusion of branches of superior or inferior mesenteric arteries often in the older age group commonly presents with sudden onset of abdominal pain and passage of bright red blood per rectum with or without diarrhoea. In the majority of cases, splenic flexure and left colon are affected. Underlying cardiovascular disease may be evident.
- On examination, the abdomen is distended and tender
- Abdominal x-ray often shows thumb printing at the site of the splenic flexure.
- Medical symptomatic management is usually adequate; surgery may be required for perforation, gangrene or stricture formation.
Comments
Post a Comment
Post Your Reply and Give Your Opinion About the Post