It is a systemic mycosis whose causal agent fungus Paracoccidioides brasiliensis. It is the most common mycosis in South America, and Brazil predominates in the South and Southeast.
Contamination occurs through the skin or aspiration. To be inhaled, fungi reach the alveoli, where they are transformed into yeast, which are the infective forms. Resistance to infection is determined by the host's ability to slow the spread fungal, and cellular immune response to the primary defence mechanism.
Signs and Symptoms:
The most affected patients are white males with a history of work in the field. Pulmonary involvement is often chronic, localized or generalized.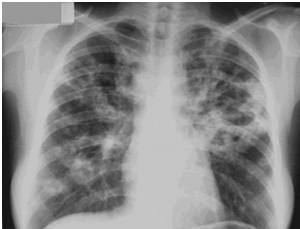
Besides the lungs, other organs can be affected, such as skin, mucous membranes, bones, lymph nodes, larynx, brain, digestive, urogenital and adrenal.
Clinically, patients present with dyspnea (shortness of breath), dry or productive cough, expectoration, hemoptysis (blood) and chest pain. Some patients also report weight loss, asthenia, fever and sweating.
Differential diagnosis:
The main differential diagnoses are tuberculosis, sarcoidosis, other mycoses, sequelae of pneumonia and cancer.Diagnosis:
The diagnosis is suspected by clinical findings and confirmed by the fungus. Other tests, such as blood count, ESR, mucoproteins and protein electrophoresis are nonspecific.Chest radiography is also very useful in the diagnosis. Generally, pulmonary changes are bilateral, diffuse, with greater involvement in the mean fields, forming an image that suggests 'butterfly wings'.
A chest CT scan allows better visualization of pulmonary involvement.
Treatment:
The treatment is done with itraconazole 100 to 200 mg daily for 6 to 12 months. As a side effect can cause nausea, dyspepsia, abdominal pain and constipation.Ketoconazole can also be used. In severe or resistant cases, amphotericin B is used.
If there is healing after treatment clinically and radiologically, serologically negative, the patient is considered cured. If serology remains positive, treatment should continue.
Prognosis:
If the diagnosis is early detection and proper treatment, the prognosis is good. However, the same does not occur when the pulmonary lesions progress to fibrosis with retraction and respiratory failure. In this case no cure for the disease, but irreversible consequences.Patients who discontinue treatment the prognosis is bad because they evolve to chronicity and spread of the disease. Death may occur due to lesions in the airways, lungs, and adrenal insufficiency.
 General medical, critical and reflective that can act with competence and scientific ethics in the health-disease through health promotion, prevention, protection and rehabilitation of the individual, family and community, through training excellence and committed to citizenship Follow her @
General medical, critical and reflective that can act with competence and scientific ethics in the health-disease through health promotion, prevention, protection and rehabilitation of the individual, family and community, through training excellence and committed to citizenship Follow her @
Comments
Post a Comment
Post Your Reply and Give Your Opinion About the Post